Arthritis
Arthritis of major joints is extremely common in Australia, with around 4 million people affected and more than 120,000 in Tasmania. The term arthritis encompasses many different causes of joint diseases, which result in pain, stiffness or dysfunction. These diseases include osteoarthritis (often referred to as wear-and-tear arthritis) and inflammatory arthritis (the most common being rheumatoid arthritis). Although arthritis can affect almost any joint in the body the joints most commonly treated by Dr. Mackie are the hip, knee, ankle, foot, shoulder, elbow and wrist.
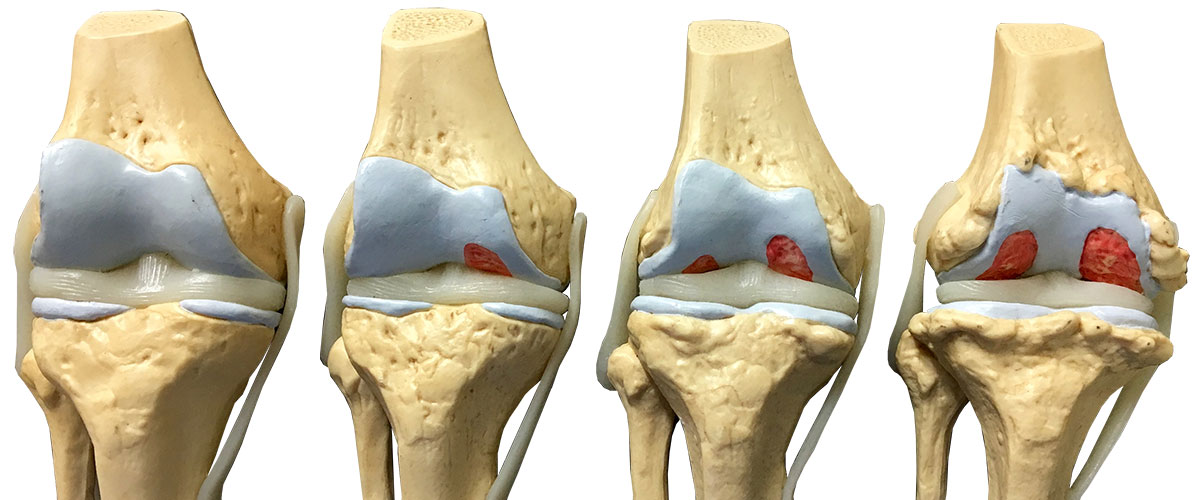
Symptoms and Presentation of Arthritis
Most patients who seek treatment for arthritis have a combination of symptoms in one or more joints. These can include:
- Pain
- Swelling
- Stiffness
- Catching
- Giving Way
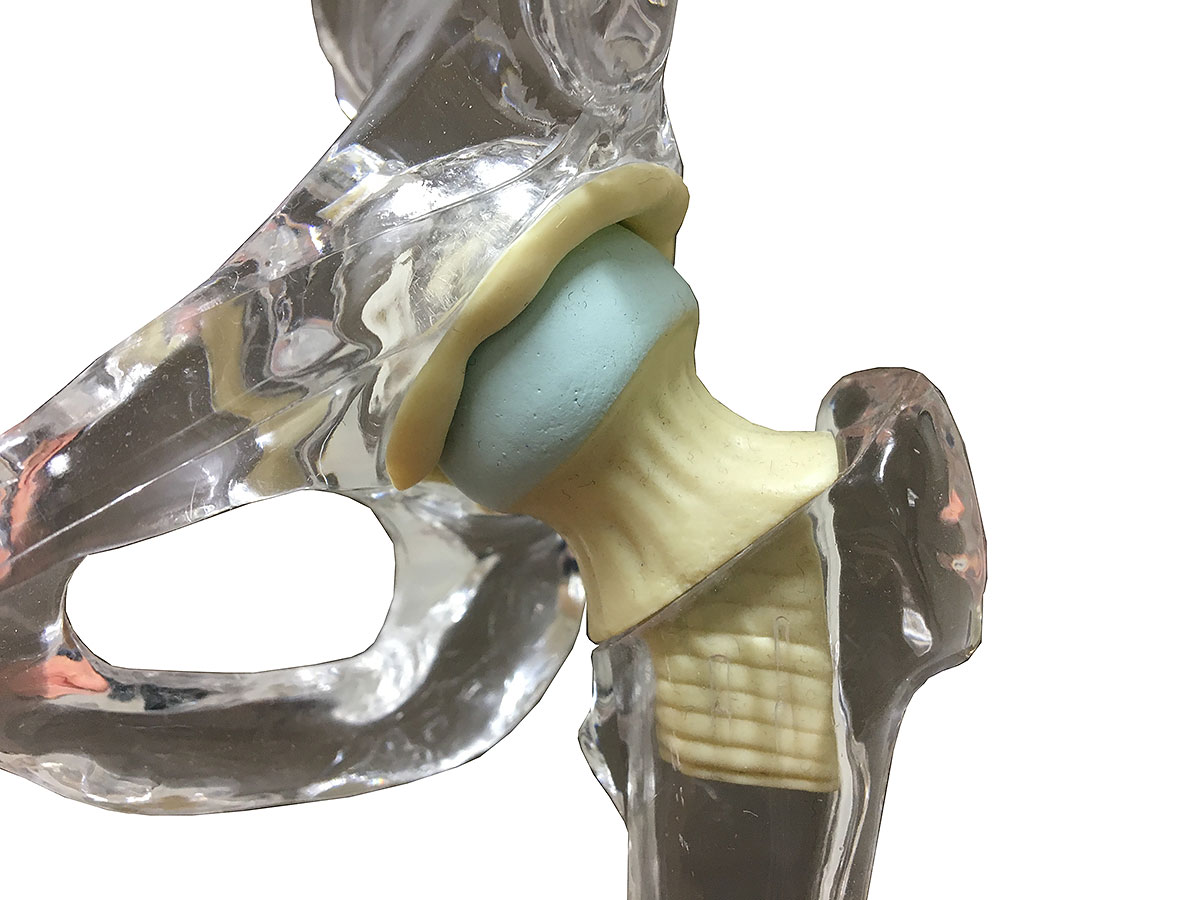

Non-Operative Treatments for Arthritis
Not all patients with arthritis require surgery. Many people are able to function at a high level with mild to moderate arthritis changes, with some people with severe arthritis (based on XRAY changes) reporting very few symptoms. Therefore it is important to consider a variety of different arthritis treatments before embarking on surgery such as joint replacement. Surgery is usually recommended only if non-surgical treatments do not help to reduce pain or improve mobility.
Weight loss
Losing excess weight will take pressure off an already diseased joint or delay progression. Patients with a Body Mass Index (BMI) greater than 35 are at greater risk of complications from surgery and all efforts should be made to reduce weight. There is very good international evidence to show that weight loss can significantly reduce symptoms in lower-limb arthritic joints. Many patients express concerns that they cannot lose weight due to an inability to exercise because of their arthritic joints. Low-impact aerobic activity needs to be trialed. Gymn-based machines such as orbital trainers / cross-trainers avoid the impact on joints associated with running or jogging. There is also good evidence to show that very few people who have a successful joint replacement go on to lose weight as a direct result of their surgery.
Walking aids
Using a walking stick can take up to 30% of the pressure from an arthritic knee joint, usually with the stick or crutch used in the opposite hand. Similarly, hip pain and limping may be reduced by helping balance the body when walking with a stick or crutch to reduce the rotation stress on muscles around an arthritic hip.
Physiotherapy
Physiotherapy can assist patients maintain range of motion and therefore functional use of arthritic joints. A physiotherapist may be able to assist some patients with taping techniques or chronic pain management techniques to reduce arthritis discomfort.
Hydrotherapy may be a very useful method of keeping arthritic joints mobile and movement against water-resistance will help with muscle strengthening.
Orthotics and braces
Orthotics or shoe wear modification that changes the pressure points across arthritic joints can be helpful for some patients. Correct fitting and supply of orthotics does require careful evaluation of limb alignment and liaison between medical practitioners and orthotic specialists (or podiatrists).
Simple elasticated braces may make some joints (especially knee and ankle) feel more comfortable and controlled. The contact of the brace with skin and muscle improves the communication between the joint and the brain, allowing for better “control” of the joint during movement and stress.
More complex (and more expensive) braces can transfer pressure from the most affected area, predominantly for knee arthritis. These braces may start at ~ $500 and go up to ~ $2,000 in cost. They should be supplied and fitted by a suitably qualified specialist (usually an orthotist).
Taking medicines may reduce pain and inflammation
Anti-inflammatories
Are commonly used or prescribed for arthritis but should primarily be used for inflammatory arthritis such as rheumatoid arthritis.
Panadol and Panadol osteo
Panadol is a very safe medication if taken at correct dosing. Panadol Osteo is a slow release form of panadol that can safely be used long-term. Panadol is often used to complement other painkillers in the early postoperative period. It may relieve the background pain of early to moderate arthritis. Dr. Mackie will rarely agree to perform joint replacement surgery if panandol osteo has not been trialed.
Fish Oils
May benefit some patients with inflammatory arthritis (rheumatoid, ankylosing, psoriatic) but there is not enough evidence to recommend their routine use in osteoarthritis. Fish oils can increase bleeding (and must be ceased a week prior to any surgery).
Glucosamine
There is mixed evidence in early knee arthritis for the use of glucosamine. It may slow down cartilage damage (but will not restore cartilage). It has been shown to have some pain-killing effects. Evidence is lacking to support glucosamine use in hip arthritis.
Prescription Pain Killers
Patients’ general practitioners are the best people to discuss long-term pain killer use and the various options, eg Tramadol, Codeine, Endone, Norspan skin patches.
Herbals
There is no high-quality research to support the use of herbal remedies in arthritis management. It is very important to not start any herbal or “complementary therapies” for arthritis without liaising with a general practitioner about potential side effects or interactions with prescription medications.
Acupuncture
May be helpful for some patients with knee arthritis but further research is required. There is less evidence for the use of acupuncture for hip arthritis.
Viscosupplementation
Occasionally - an injection into the joint (Hyaluronic acid) can change the chemicals in the knee and reduce pain. The cost of this injection is ~ $480 (2016) and is not covered by Medicare or private health funds. There is inadequate evidence to support the use of viscosupplementation in other joints.
Other Surgery Options
Depending on the symptoms and circumstances in each individual case, there may be surgical alternatives to having a joint replacement. These might include an operation to reshape the bones. Re-aligning the leg via an operation (osteotomy) may transfer weight-bearing from a diseased portion of a joint to an area of better quality cartilage. Rarely an arthrodesis (a surgical procedure that permanently fuses the joint together) may be required.
Arthroscopy (Keyhole Surgery) For Arthritis
Arthroscopy surgery is relatively safe, but if cartilage damage is widespread within an arthritic knee then debridement (cleaning of rough edges etc.) has been shown to have very little long-term benefit. Arthroscopy in the setting of arthritis should only be performed for very specific mechanical symptoms, such a catching / locking / sharp knee pains. There is unlikely to be any reduction in background pain or longstanding pain.
Most international studies into hip and knee arthritis have demonstrated that joint replacement surgery provides significant immediate and long-term benefits for patients when good selection criteria are used to proceed to surgery.
